No Effort Required
Time To Dig Up Dead Relatives
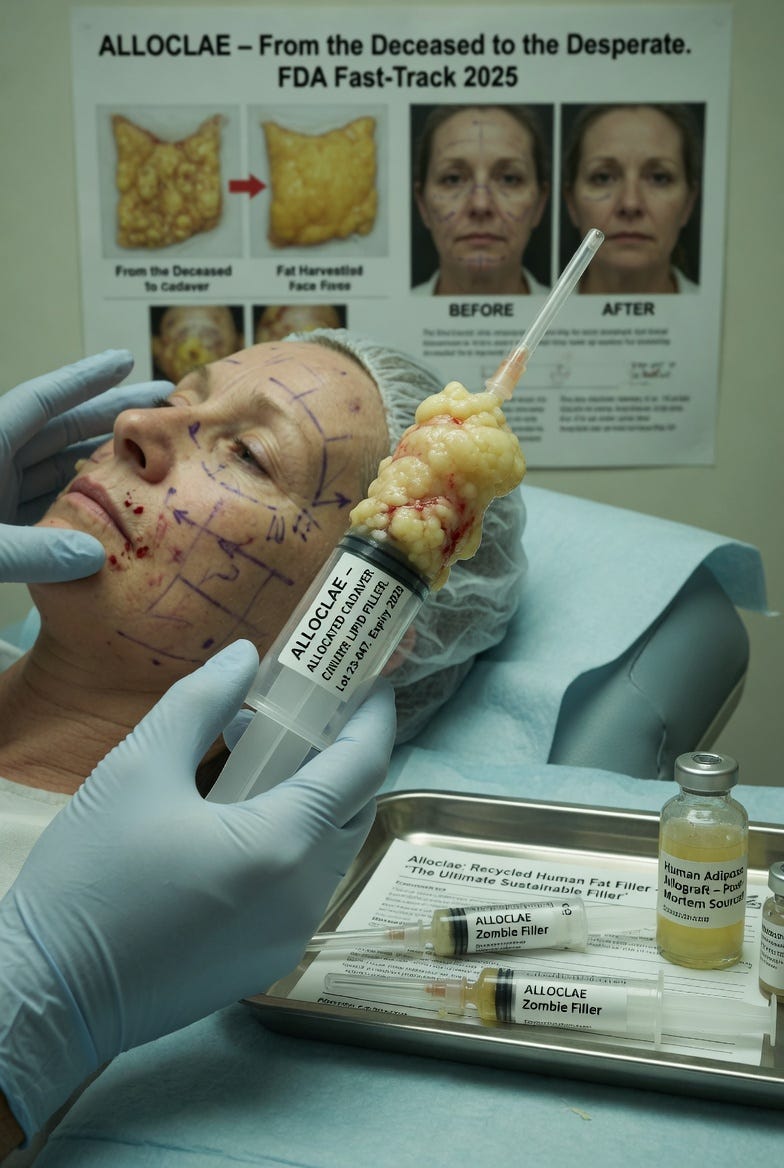
In late March 2026, The Guardian published a dispatch that reads like satire until one realizes it is not. Titled with the wry observation that men can now “say he went to the gym” after a simple injection, the piece introduces Alloclae: sterilized, purified fat harvested from cadavers and packaged for cosmetic use. Marketed as “zombie filler,” this allogeneic adipose tissue is injected into pectorals, breasts, buttocks, or any area one wishes to augment. No liposuction, no general anesthesia, no meaningful recovery. One leaves the clinic and resumes the day with a newly contoured body assembled, quite literally, from the remains of the dead.
The procedure is presented as a logical response to another modern convenience: GLP-1 receptor agonists such as Ozempic and its successors. Rapid weight loss has left many patients with diminished fat stores precisely where they once desired volume. Alloclae fills the gap without requiring patients to regain the weight or undertake the disciplined regimen of resistance training and caloric surplus. It is, in the words of the surgeons interviewed, a “gamechanger” for those who lack sufficient autologous fat or simply prefer not to exert themselves. A 68-year-old patient receives 100 cubic centimeters in his chest and walks out looking as though he has spent months in the weight room. A woman post-Ozempic restores her silhouette in under an hour. Instant gratification, no sweat equity required.
In a prior article “Ramadan or Ozempic?,” I have already examined the cultural preference for pharmacological shortcuts over sustained discipline. That essay argued that fasting during Ramadan cultivates not only metabolic resilience but also humility, patience, and self-mastery—qualities a weekly injection cannot confer. Alloclae extends this logic to its terminal conclusion. If one can outsource weight loss to a syringe, why not outsource muscle definition and youthful contours to the tissue of dead strangers? The body becomes a project to be optimized rather than a vessel to be stewarded through effort.
This development is not merely a medical novelty; it is a cultural symptom. Contemporary beauty standards, amplified by social media and the “looksmaxxing” subculture, demand visual perfection with minimal visible labor. The gym, once a temple of delayed gratification, now competes with procedures that allow individuals to claim the aesthetic of discipline without having practiced it. One need not track macros, endure soreness, or confront the monotony of progressive overload. One simply schedules an appointment, pays the fee—often tens of thousands of dollars for meaningful volume—and lets the technician do the work. The corpse supplies the raw material; the patient supplies only the credit card.
The ethical dimensions are equally disquieting. Fat is harvested from tissue banks certified by the American Association of Tissue Banks. Donors, or more accurately their next of kin, sign general consent forms that rarely specify the ultimate cosmetic destination of their adipose tissue. The dead have no say in whether their remains will be repurposed to enhance a stranger’s pectorals so that he may appear, in photographs at least, to have lived a life of physical rigor. Philosophically, this commodifies mortality in service of vanity. We have long accepted organ donation to save lives; we now contemplate fat donation to improve selfies. The distinction between life-saving allograft and life-enhancing filler collapses when convenience is the highest value.
Critics within the medical community, including Dr. Glenn Lyle, have noted the absence of robust long-term data. Early adopters accept the risk of oil cysts, granulomas, or imaging complications that may complicate future breast-cancer screening. Yet the market moves faster than the evidence. Regulatory oversight treats human fat as a familiar biologic rather than a novel cosmetic device, creating a lighter approval pathway than that required for synthetic fillers or implants. The result is a gold-rush atmosphere in which innovation outpaces prudence.
One might counter that Alloclae is merely another tool in the aesthetic arsenal, akin to Botox or hyaluronic acid. The difference lies in its origin. Synthetic or autologous materials do not implicate the dignity of the deceased. Here, the boundary between life and death is crossed for reasons that are fundamentally elective. The procedure invites us to ask what, precisely, we are optimizing. Is the goal a healthier body or merely the appearance of one? Does the pursuit of effortless beauty ultimately erode the very qualities—resilience, authenticity, self-respect—that make human flourishing meaningful?
This is not an argument against compassion for those who struggle with body image. Modern life already imposes enough pressures without adding moral condemnation for personal insecurity. Yet compassion should not preclude clear-eyed cultural critique. When entire industries profit by promising transformation without transformation, we must interrogate the message being sold. The promise of “no effort required” quietly undermines the quieter satisfactions of effort well spent: the quiet pride of incremental progress, the camaraderie of shared struggle, the integrity of a body earned rather than purchased.
The article concludes with patients who express mild discomfort—“It’s a little bit strange to think about”—before proceeding anyway. That hesitation is the last remnant of an older moral intuition. Once normalized, even that discomfort will fade. Future generations may view cadaveric filler as unremarkable as collagen or silicone. The question we must ask ourselves today, while the strangeness still registers, is whether a life assembled from the effortless and the borrowed is one we truly wish to inhabit.



We are living in some wild times